GI Bleed
Avoid excessive crystalloid resuscitation - Anand Swaminathan
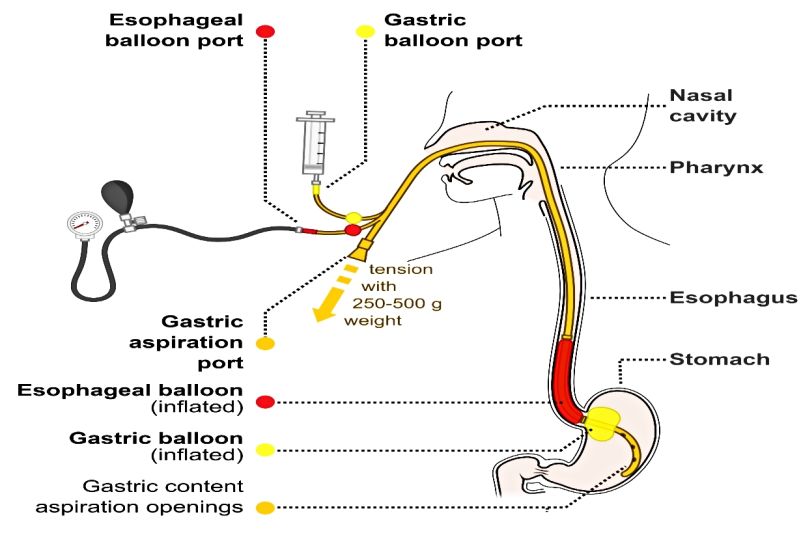
image by: Olek Remesz
HWN Recommends
Massive GI bleed management
Give blood. Don’t waste time on crystalloid fluid boluses. The patient is losing blood, they need blood replaced. Start with type O, and change to type specific as soon as possible. I won’t get into the debate about different transfusion ratios here. Just use whatever protocol your institution has, give lots of blood, and make sure you have more ready when needed.
Almost everyone has heard that we should be transfusing less and aiming for a lower hemoglobin target in GI bleeds. However, patients were excluded from that study if they had “massive exsanguinating bleeding” – so ignore the evidence here, and just get blood on board.
Resources
 Gastrointestinal haemorrhage
Gastrointestinal haemorrhage
GI haemorrhage is divided into upper GI haemorrhage and lower GI haemorrhage based on the underlying cause and differences in the approach to management.
 Gastrointestinal Bleeding: The Next Frontier (for TXA)
Gastrointestinal Bleeding: The Next Frontier (for TXA)
TXA has been shown to improve outcomes in cases of bleeding including postpartum hemorrhage (WOMAN trial), trauma (CRASH-2 trial), epistaxis, oral bleeding and even inhaled TXA for hemoptysis (shout out to Dr Bogach for a recent case of this). It’s low rate of complications (remember its antifibrinolytic, NOT prothrombotic) makes it a great choice for controlling bleeding.
 No Reason Not to Use TXA for Critical GI Bleeds
No Reason Not to Use TXA for Critical GI Bleeds
Octreotide and ceftriaxone are quickly delivered. Proton pump inhibitors are lambasted for their lack of efficacy yet dutifully ordered despite compelling evidence of no benefit and even a signal of harm. We evidence-based clinicians know the literature, and we cling to transfusion trial talismans as we seek to stem the tide of dark blood that seems to flow as quickly as we can replace it. Curiously, one medication has remained inexplicably absent from our routine resuscitation of the critically ill GI bleeder. Tranexamic acid, or TXA...
 Tranexamic Acid for GI Bleeds
Tranexamic Acid for GI Bleeds
Tranexamic acid (TXA) is an antifibrinolytic agent that has been studied in the management a variety of hemorrhagic conditions, including trauma, epistaxis, postpartum hemorrhage, and intracerebral hemorrhage. Its use in gastrointestinal (GI) bleeding has been studied fairly extensively, and a Cochrane systematic review from 2014 found that TXA conferred a beneficial effect on mortality, with the caveat that additional research was still needed before this could be said with any certainty.
GI Bleeding
Active bleeding is obviously worrisome. Hematemesis is more worrisome than hematochezia, because upper GI bleeding carries a higher mortality than lower GI bleeding.
GI Bleeds
All right folks, the chief complaint we all know and love: “rectal bleeding”. It may strike fear in your heart or bring you comfort in its algorithmic approach. However, GI bleeds can present in a variety of ways from the “sick” to “not sick”. So, grab your GUAIAC cards and let’s get started.
Anticoagulants and GI Bleed with Walter Himmel
... we have Dr. Himmel telling us the story of his Best Case Ever on anticoagulants and GI bleed. He discusses the most important contraindication to DOACs, the importance of not only attempting to reverse the effects of anticoagulants in a bleeding patient but managing the bleed itself and more great pearls.
Aspirin and Vitamin C Together at Last
Aspirin side effects kill about a thousand people a year in the US. If aspirin were a new drug, it would have a tough time getting approved by the FDA and would only be available by prescription.
Diagnosis of gastrointestinal bleeding: A practical guide for clinicians
This review summarizes the overall diagnostic approach to gastrointestinal bleeding and provides a practical guide for clinicians.
EM@3AM: GI Bleed
The importance of reviewing the medication list cannot be overstated: Aspirin, NSAIDs, anticoagulants, and glucocorticoids all increase the risk of bleeding. Medications such as beta-blockers can blunt a tachycardic response.
Episode 101 GI Bleed Emergencies Part 1
Join Anand Swaminathan, Salim Rezaie and Jeannie Callum to discuss the management of some of our most challenging GI bleed emergencies. In this Part 1 of our two part podcast on GI bleed emergencies we answer questions such as: How do you distinguish between an upper vs lower GI bleed when it’s not so obvious clinically?
Episode 102 GI Bleed Emergencies Part 2
In Part 2 of our two part podcast on GI Bleed Emergencies Anand Swaminathan and Salim Rezaie kick off with a discussion on the evidence for benefit of various medications in ED patients with upper GI bleed. PPIs, somatostatin analogues such as Octreotide, antibiotic prophylaxis and prokinetics have varying degrees of benefit, and we should know which ones to prioritize.
 Massive GI bleed management
Massive GI bleed management
Don’t waste time on crystalloid fluid boluses. The patient is losing blood, they need blood replaced. Start with type O, and change to type specific as soon as possible. I won’t get into the debate about different transfusion ratios here. Just use whatever protocol your institution has, give lots of blood, and make sure you have more ready when needed.
Society for Academic Emergency Medicine (SAEM)
The differential diagnosis of GI bleeding is generally categorized into Upper or Lower GI Bleeds, based on whether the bleeding occurs anatomically above or below the Ligament of Treitz. Bleeding from the Upper GI tract is 4 times more common than bleeding from the Lower GI tract.

Introducing Stitches!
Your Path to Meaningful Connections in the World of Health and Medicine
Connect, Collaborate, and Engage!
Coming Soon - Stitches, the innovative chat app from the creators of HWN. Join meaningful conversations on health and medical topics. Share text, images, and videos seamlessly. Connect directly within HWN's topic pages and articles.













