Endocannabinoid System
The endogenous cannabinoid system, named after the plant that led to its discovery, is perhaps the most important physiologic system involved in establishing and maintaining human health - Dr. Dustin Sulak
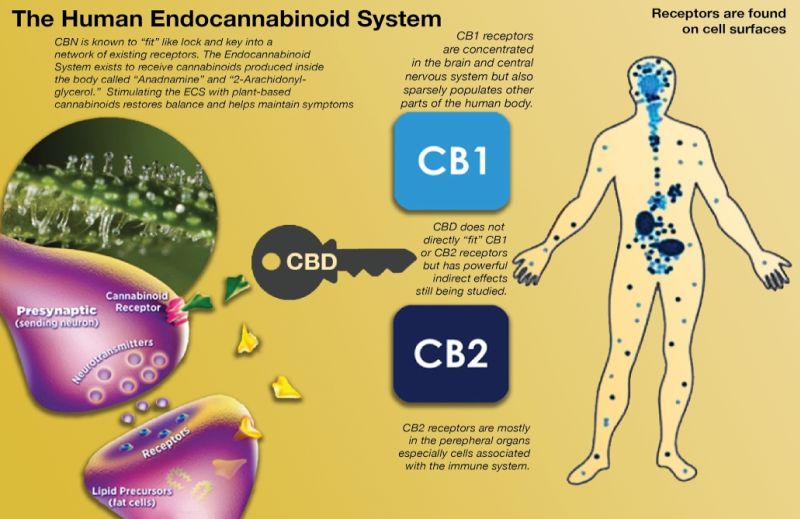
image by: Terpenes
HWN Recommends
The endocannabinoid system: Essential and mysterious
Many of us have heard of some of the transmitter systems within our bodies, such as the sympathetic nervous system, which gives us our fight-or-flight response. Fewer have heard of the more recently discovered endocannabinoid system (ECS), which is amazing when you consider that the ECS is critical for almost every aspect of our moment-to-moment functioning. The ECS regulates and controls many of our most critical bodily functions such as learning and memory, emotional processing, sleep, temperature control, pain control, inflammatory and immune responses, and eating. The ECS is currently at the center of renewed international research and drug development.
What is the ECS?
The…
Resources
Introduction to the Endocannabinoid System
The endocannabinoid system, with its complex actions in our immune system, nervous system, and all of the body’s organs, is literally a bridge between body and mind. By understanding this system we begin to see a mechanism that explains how states of consciousness can promote health or disease.
Med schools need to get with the times on medical marijuana, chronic pain, and more
In a study published last fall, researchers found that fewer than 1 in 10 medical schools included medical marijuana in their curricula. Two-thirds of medical school deans reported that their graduates “were not at all prepared to prescribe medical marijuana,” and a quarter reported that their graduates “were not at all prepared to answer questions about medical marijuana.”
Old dope, new tricks: the new science of medical cannabis
In fact, cannabis science is one of the fastest moving frontiers in pharmacology and has accelerated by the realisation that we’re all already marinated in cannabis-like molecules (endocannabinoids) and their receptors. Endocannabinoids help regulate many physiological processes: mood, memory, appetite, pain, immune function, metabolism and bone growth to name a few (there are even cannabinoid receptors in sperm).
The Brain Produces Its Own Version of THC
By studying how weed affects us, researchers got a much better sense of how the body functions when not under the influence of tetrahydrocannabinol (THC), the main active ingredient in cannabis. Because, it turned out, the endocannabinoid system wasn't just lying dormant waiting for THC to enter the body. It's working all the time. And, as one paper put it, "the endocannabinoids are literally a bridge between body and mind."
The Endocannabinoid System, Cannabinoids, and Pain
Only recently have we gleaned scientific insight into several of the pharmacologically distinct cannabinoids and their effects at specific receptors within various animals and humans.
The Endocannabinoid System, Our Universal Regulator
ECS is a unique system in multiple dimensions. To begin with, it is a retrograde system functioning post- to pre-synapse, allowing it to be a “master regulator” in the body.
The Endogenous Cannabinoid System: A Budding Source of Targets for Treating Inflammatory and Neuropathic Pain
An overwhelming body of convincing preclinical evidence indicates that cannabinoids produce antinociceptive effects in inflammatory and neuropathic rodent pain models. Cannabinoid receptor agonists, endocannabinoid-regulating enzyme inhibitors, and other pharmacological strategies to manipulate the endogenous cannabinoids system decrease the hyperalgesia and allodynia induced in diverse inflammatory and neuropathic pain states.
The Science of the Endocannabinoid System: How THC Affects the Brain and the Body
After several decades of research, scientists studying the effects of marijuana made several important discoveries. Not only did they identify the active ingredient in marijuana, they also discovered where and how it works in the brain—via a new system they called the endocannabinoid (EC) system. The EC system—named after the marijuana plant Cannabis sativa and its active ingredient delta-9-tetrahydrocannabinol (THC)—is a unique communications system in the brain and body that affects many important functions, including how a person feels, moves, and reacts.
How (and Why) Your Brain Makes Its Own Cannabinoids
First identified in the late 1980s, the so-called endocannabinoid system consists of CB1 receptors predominantly located in the nervous system, connective tissues, gonads, glands, and organs; and CB2 receptors, primarily found in the immune system and also present in the spleen, liver, heart, kidneys, bones, blood vessels, lymph cells, endocrine glands, and reproductive organs.
 The endocannabinoid system: Essential and mysterious
The endocannabinoid system: Essential and mysterious
Study of the ECS was initially focused on attempts to understand (and demonize) an illegal drug, but new research has since flourished into a far more broad-based exploration into what is an astoundingly intricate and far-reaching system by which our bodies learn, feel, motivate, and keep themselves in balance.
Top 10 Ways to Support the Endocannabinoid System
The ECS is perhaps most notable for its role in regulating the limbic system, a part of the brain responsible for emotions, motivation, and our stress response. This system responds to our body’s own endogenous cannabinoids, anandamide and 2-AG, and to exogenous cannabinoids.
Canntelligence
Canntelligence will transform consumers and healthcare practitioner’s understanding of the endocannabinoid system and science of the cannabis plant.

Introducing Stitches!
Your Path to Meaningful Connections in the World of Health and Medicine
Connect, Collaborate, and Engage!
Coming Soon - Stitches, the innovative chat app from the creators of HWN. Join meaningful conversations on health and medical topics. Share text, images, and videos seamlessly. Connect directly within HWN's topic pages and articles.













