Stroke - Is the Treatment Worth the Risk?
James L. Jones | Insider
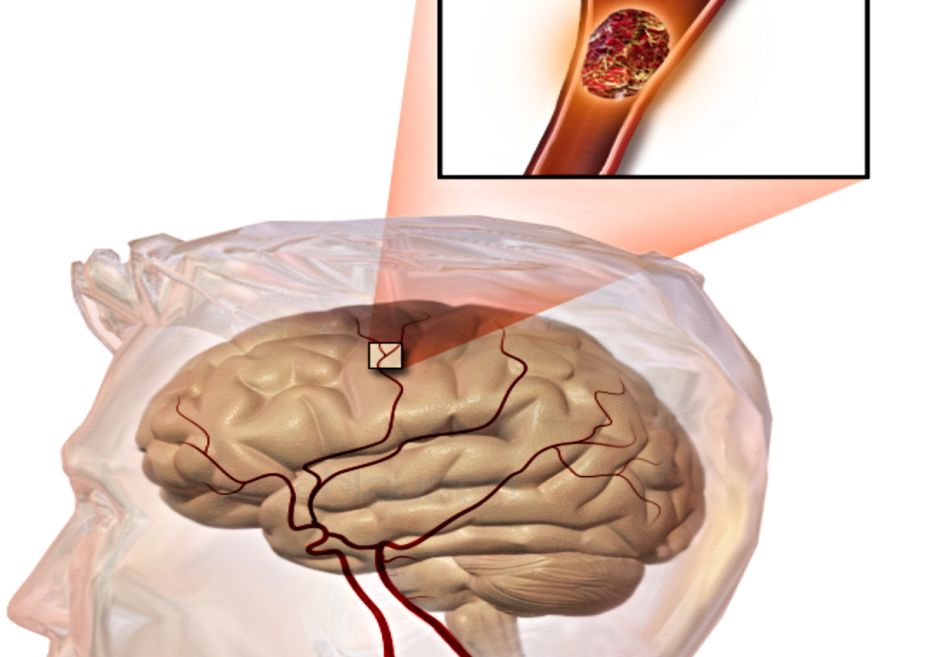
image by: Blausen Medical Communications, Inc.
It's sad to say that customary stroke treatment is similar to how heart attacks were treated before the 1970's. New technology is needed, not just clot busters. In the meantime know where the nearest stroke treatment center is
Eighty-five per cent of strokes are caused by blockages or clots as opposed to a bleed and there are 700,000 new strokes diagnosed every year. Most of the patients live. However CVAs are responsible for 160,000 deaths in the U.S. which represents the third leading cause of death. Heart disease is still the leader at about 650,000 a year and cancer is gaining on heart disease but still is second at 560,000 deaths every year. The incidence of strokes went down all through the seventies and eighties, reaching a low point in 1992 of just under 140,000. But since then it has gone up, and will continue to rise.
Boomers are getting old. Which is why in the U.S. strokes are the leading cause for dollars spent for treatment of long-term disability which represents forty five billion dollars of the total health care expenditures of 2.7 trillion dollars. Nothing else even comes close. To have so many dollars spent on rehabilitation of a disease makes one wonder about what kinds of treatment are available.
Unfortunately there is no current acceptable, effective or accessible treatment for stroke.
It’s true! There is no treatment for stroke other than those available at a few research centers. The majority of stroke patients thruout the world get what we call supportive care. And they get a lot of rehabilitation and many stay disabled for life. In fact it is sad to say that customary stroke treatment is similar to how heart attacks were treated before the 1970's. Care givers would simply stand by and give supportive care.
Since then, we have witnessed major advances in heart disease management including the use of angioplasty, stents and various other options which are widely available in most countries, whereas the only major advances in stroke treatment in the past two decades are related to thrombolytic use, which is not saying much. Thrombolytics have shown an improvement in neurologic outcome but at the same time have shown an increased risk for intracranial bleeding which can result in a poor outcome including death as opposed to the possibility of just chronic disability from the initial stroke.
The rationale in the first place for using a treatment that can be worse than the disease has been based on the following landmark studies.
NINDS (National Institute for Neurologic Disorders and Stroke rt-PA Stroke Study Group)
Actually done in 1995, this was the hallmark study which proved, to it’s advocates, that ischemic stroke could be treated effectively and safely with TPA, or Tissue Plasminogen Activator, one of the first clotbusters. It was done using a very strict protocol. In fact, only two per cent of potential candidates were accepted into the study. No patients with symptoms more than two and a half hours were accepted and all patients had CT scans read by a radiologist-specialist to make sure the strokes were truly from clots and not bleeding.
The authors of this study suggested they had found a successful treatment when their results were published. Forty per cent of patients had flow reestablished, the clot dissolved, 15% of these patients had a reoclussion and outcomes at three months were better.
Here’s the catch, six percent of patients had bleeding from the treatment; the clotbuster actually caused bleeding and more damage. Untreated patients had bleeding less than one percent of the time. And mortality for TPA treated group was the same as the untreated group, about eighteen per cent. It wasn’t known at the time, but around one or two percent of all ischemic, clot-associated, stroke patients will actually develop bleeding within the first day or two following their CVA because of the initial damage to the artery.
It’s also possible that the strokes were actually hemorrhagic from the beginning and that the bleeding was so small it didn’t show up till later. Advocates for thrombolytic therapy claimed it was an acceptable risk since mortality was the same for both groups and the neurologic improvement was so much more in the treated group, thirteen per cent, using a specialized neurologic function scoring system.
NINDS actually failed to achieve it’s primary treatment goal of an immediate improvement in neurologic function. But the three month function assessments showed improvement with the TPA, and this was the basis for approval of the subsequent studies. And there were a lot of them.1
STARS (Standard Treatment with Alteplase to Reverse Stroke)
Actually had better results than NINDS, only three per cent of treated patients had bleeds and overall mortality was about half that of the control or untreated group, thirteen percent. It used a different thrombolytic, Ateplase, and kept the same rigid entrance requirements for the study, including no patients with symptoms more than two and a half hours.2
PROACT II (Prolyse in Acute Cerebrovascular Thrombosis)
To avoid the bleeding complications of the large doses of intravenously administered thrombolytics, researchers injected small doses at the clot-blockage through catheters they threaded up the arteries. Sixty six per cent of the blockages opened up and a small number reoccluded, but the bleeding rate was ten per cent. A definite plus: Patients treated up to six hours after symptoms began had improved neurological outcomes as compared to the NINDS patients.3
ECASS, ATLANTIS and others (European Cooperative Acute Stroke Study, Alteplase Thrombolysis Trail)
Some of these and other studies were done in Europe, others here in Cleveland, and at Yale. Researchers expanded the acceptability requirements for the study. Patients with symptoms for up to six hours were included, and researchers increased the dosages of the TPA. Results for obtaining reperfusion was about the same; thirty percent of the patients had reflow, a third of those reoccluded. But the mortality increased to twenty five per cent at one of the centers, and bleeding increased to anywhere between twelve to twenty two percent.
Critics pointed out that results with the higher doses were essentially the same as with NINDS, and that the bleeding rates made the higher dosages prohibitive. And the twenty-five percent mortality rate was definitely unacceptable. The concept of larger doses was in disfavor and researchers started to suspect that brain arteries were quite fragile and more subject to rupture if the time to reestablishing blood flow was longer. 4,5
CASES (Canadian Activase Stroke Effectiveness Study)
A Canadian study later confirmed the NINDS findings and had a low bleeding rate of four and a half per cent and still achieved the favorable neurologic improvements with treatment. It was a large study, using 1130 patients.6
So, is the current treatment worth it?
Roughly six percent OR one out of every twenty stroke patients will be perhaps worse off because of their treatment. Risk factors for bleeding include larger areas of stroke, more severe symptoms (unconscious), older patients, patients with low platelets for whatever reason, people with high blood sugar or a history of diabetes or congestive heart failure.
We’re at that point in stroke treatment, waiting for technology to help us treat a difficult disease similar to where heart attacks were before the advent of specialized invasive procedures. TPA was the first commonly used effective thrombolytic, and it saved thousands of lives, but also it had a bleeding rate of three to five percent. About one out of every twenty patients would have a hemmorhagic stroke as a complication to the TPA treatment and it was usually in older patients with risk factors for stroke. However, the risk of bleeding was considered acceptable given the drug’s dramatic effectiveness, until other treatment modalities came along.
Additionally there are also other challenges to developing a safe and effective treatment for stroke.
Only two per cent of the patients initially suspected of having a stroke would actually qualify for the treatment. That’s not a lot of patients to justify having all these resources on hand. One/third of all suspected stroke patients are what are known as “mimics.” The patients at first appear to have had a stroke but eventually turn out to have TIAs, or temporary strokes, low blood sugar, tumors, thyroid disease, or seizures.
A further problem is that TIAs, the most commonly presenting Mimic, is defined by some experts as lasting for forty-eight hours. That means the symptoms could just go away on their own in two days. What if you treat a TIA that would have gotten better and the patient has a hemmorhagic stroke?
The ideal patient is a middle aged person, still awake, who knows the minute he felt different, with few other health problems, and able to understand the risks of treatment. However most of the excluded patients simply don’t know when their symptoms started. Sadly, most stroke symptoms are not noticed when the stroke first happens. Many patients are sleeping, a lot are older and unattended at the time. The usual story is “Well, Grandpa seemed OK Easter Sunday when we came over, but now he’s just not right.”
Let's examine what's in the pike.
Development of regional stroke centers
Actually, there are currently a few stroke centers in the U.S. aligned with a prehospital care system with protocols for screening potential patients and directing them to the stroke center, bypassing other hospitals.
In addition to an emergency physician, there would be a specially trained neuro-radiologist and a neurologist either in house or within thirty minutes of the hospital. The goal would be to administer the lysis treatment within usually three hours, although this may change as new treatments develop. The reality is, with time being such an important factor, a center with 24 hour resources has to be available within a short time from the beginning of symptoms. Unfortunately there are not too many hospitals that can meet this criteria in addition to the few university centers that are also using other modalities in stroke management.
Community Awareness Programs
Specialized programs are sprouting up. Much as early recognition of heart attack symptoms has saved countless lives, early recognition of stroke would help get patients to the hospital within that three hour limit. There are a handful of assessment tools; STR, ROSIER and others and they all use simple measures to assess strength in the arms and legs, range of motion of the eyes, cognition and speech.
Imaging studies
Radiologists have developed better imaging techniques to accurately determine when an ischemic stroke may have happened. This would help to rule out patients with strokes more than three hours old, and rule in patients for treatment if the stroke occurred less than three hours before.
Invasive Procedures
The most exciting developments are in the area of more invasive treatments. The relatively new subspecialty of Invasive Radiology is testing some new tools. Use of tiny intra-arterial ultrasound probes to actually go to the area of blockage and dislodge the clot are being tested. Some researchers are following the ultrasound treatment with small doses of thrombolytics, mechanical retrieval of the clot, or the use of coils or stents.
One tool, known as the Penumbra Device is currently being tested and appears to open up the blocked brain vessel eighty percent of the time, and can be used up to four and a half hours after symptoms began. Some centers are trying to simply use suction to remove the clot, followed by coils. These invasive treatments are achieving reperfusion more than half of the time with minimal bleeding complications and reocclusions.
There are other promising tools being studied and developed. Most deal with snares, stents, and suction devices. The MERCI trial is testing a snare that reportedly opens up the vessel eighty per cent of the time and has less than five percent bleeding complications, most of which are minor and asymptomatic.7
Non Invasive Procedures
One interesting treatment uses an externally directed ultrasound wave to disrupt the clot followed by administration of clotbusters. The blood vessels open up about half the time. This is a treatment that could conceivably be administered at a community or rural hospital without the need for a time-consuming transfer to a stroke center.
What can you do now?
Risk modification can help to prevent stroke.
Everyone, especially those at risk, should know where the nearest stroke centers are in your community. Also contact your county’s Department of Health Services and ask if the paramedics have a screening protocol for strokes and if they can transport directly to a stroke center.8
Raise awareness in your community and among your friends. Contact your nearest stroke center and ask for someone to give a talk to your church group, community service club, schools. If you take or sponsor CPR courses, make sure stroke recognition is included in the curriculum.
The Bottom Line
Despite the potential for intracranial bleed and even death physician-advocates and drug companies continue to campaign for the wider use of thrombolytics in the treatment of stroke and are advocating establishing stroke centers, with 24 hour resource coverage.
One gets the impression that within the next few years a combination of technological advances and community awareness will start to reduce stroke mortality and morbidity. However, any effective treatment for stroke will have to find a way to extend the treatment time window for those patients who do not live within a few minutes of a stroke center.
There is no good criteria, at this point in time, advocated for choosing which patients to treat other than having the treating physician ask himself “If this were me would I want to live with this disability, or take the risk of being worse off with the treatment.” A rather subjective criteria. But the reality is, many patients are senile to one degree or another, older, have multiple other health problems, and nobody knows when the symptoms started.
While we all wait for the expected advances in stroke treatment, be prepared for the day when you or a loved one may have to make your decision to treat an acute stroke with thrombolytics. Under what circumstances would you be willing to take the risk and when would it be worth the risk?
Published June 29, 2009, updated August 14, 2012
References
- NINDS rt-PA Stroke Study Group, National Institute for Neurologic Disorders and Stroke, 1995
- STARS, Standard Treatment with Alteplase to Reverse Stroke, 2000
- PROACT II, Prolyse in Acute Cerebrovascular Thrombosis, 1999
- ECASS, European Cooperative Acute Stroke Study, 1995
- ATLANTIS, Alteplase Thrombolysis Trial, 1999
- CASES, Canadian Activase Stroke Effectiveness Study, 2005
- MERCI, Mechanical Embolus Removal in Cerebral Ischemia, 2004
- The Internet Stroke Center
Further reading and resources
- Stroke for Dummies, Marler, John R., 2005, Lifestyles Paperbacks
- National Stroke Association
J. Linder Jones MD MHA practiced emergency medicine for over two decades in Southern California and now writes on occasion for HealthWorldNet.

Introducing Stitches!
Your Path to Meaningful Connections in the World of Health and Medicine
Connect, Collaborate, and Engage!
Coming Soon - Stitches, the innovative chat app from the creators of HWN. Join meaningful conversations on health and medical topics. Share text, images, and videos seamlessly. Connect directly within HWN's topic pages and articles.